Most of the time, we do not get to speak to our doctors enough to obtain adequate information about a condition, diagnosis or whether having or not having surgery is a good option. What do we do? We search online, we ask others who underwent similar surgery, and try to make a decision. There is no turning back when we go with the surgical option so it is important to look into possible outcomes and factor in benefit vs. possible risk ratios. Pain and disability can be very overwhelming and may be the reason to push one to want surgery immediately, however it is also important to ask questions such as;
- What are the possible cons/risks of the surgery?
- What are the possible pros of the surgery?
- How long am I going to get a relief for? Will the surgery eliminate my pain or after couple years of relief, will my pain more likely to reoccur?
- What will the post surgical month be like?
- When can I go back to my daily routine?
 It is really important to make the connection between what your condition is and what the possible outcomes are to make an informed decision and take an active part in your health care. Rushing to make a surgical decision without proper education or sufficient information is not advisable and one of the tools that can ease your decision process is Decision Aids.
It is really important to make the connection between what your condition is and what the possible outcomes are to make an informed decision and take an active part in your health care. Rushing to make a surgical decision without proper education or sufficient information is not advisable and one of the tools that can ease your decision process is Decision Aids.
Shared decision making is a collaborative process that allows patients and their providers the ability to make health care decisions together, taking into account the best scientific evidence available, as well as the patient’s values and preferences1. Decision aids are tools that help patients understand their health condition, the available options for screening or treatment, and the possible outcomes of those options by providing patients and their families with unbiased, evidence-based information. The program compares nonsurgical treatments, such as lifestyle changes, exercise therapy, medications such as NSAIDs, injections, and complementary and alternative therapies to different surgical options for that condition. It also underlines important considerations, such as rehabilitation and timing of surgery, as well as provides interviews with real patients about their experiences and interviews with two orthopedic surgeons.
 Decision aids consist of but are not limited to back care programs, breast and prostate cancer programs, chronic condition programs such as coronary heart disease and diabetes, orthopedic programs such as torn meniscus of the knee, arthritis of the knee, herniated disc, spinal stenosis, osteoporosis and so on. Each decision aid is overseen by a medical editor who
Decision aids consist of but are not limited to back care programs, breast and prostate cancer programs, chronic condition programs such as coronary heart disease and diabetes, orthopedic programs such as torn meniscus of the knee, arthritis of the knee, herniated disc, spinal stenosis, osteoporosis and so on. Each decision aid is overseen by a medical editor who
has published research in the topic area, clinical input comes from a team of clinical advisors representing key specialties for patient care, and from patient focus groups who offer input. Decision aids do not replace counseling from a health care professional, only complement and facilitate the decision process for the patient1.
2011 study by Stacey et al2, a systemic review of eighty-six randomized trials, concluded that patients participated more in decision making because their knowledge on the possible benefits and harms of the treatment options have been improved. Decision Aids are likely to cause a positive effect on communication between the patient and the provider and appear to reduce the choice of surgery when patients are informed about other treatment choices. Decision Aids have a variable effect on actual choices and on the time patients require for consultation, and have no adverse effects on health outcomes or satisfaction.
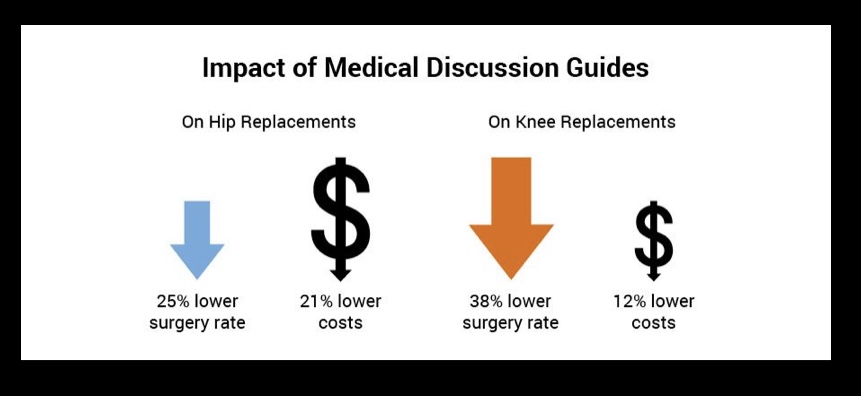
2012 observational study by Artenburn et al3 examined the associations between introducing decision aids for elective hip and knee replacement, changes in rates of surgery and costs of care using a pre-post design. They found that video-based decision aids for knee and hip osteoarthritis in a large, multisite orthopedic group practice settings was associated with a 38% reduction in knee and 26% reduction in hip replacement surgeries during a 180-day period. They found a 12–21% reduction in 180-day costs of care for patients with knee and hip osteoarthritis. These findings are consistent with results from randomized studies of decision aids, which have suggested that decision aids may lower the use of elective surgery, at least in the short term3.
Decision aids typically include a brochure, pamphlet, video or website and more information can be accessed through http://informedmedicaldecisions.org
A note for future DPTs and DPTs,
We are all aware that there is not enough time spent on patient education. Even though there is some overlay within health care professions, one would expect that patients would be given information regarding their condition from different sources. Unfortunately, this is not the case. With PT moving to a doctorate level and having “true” direct access in many states, it is vital for each one of us to pay a great deal of attention to patient education and stop assuming that the patient was provided with an explanation about their condition from their doctor. What we are taught in classrooms regarding care management can differ from what goes on in real world. In order to live up to the high standards we are presented in our DPT programs across the country and take our profession to a more noble level, we have to increase our emphasis on evidence-supported research. Backing up our treatments with evidence, and educating our patients on their condition will help us advocate for ourselves as well as provide what is best for our patients.
References
1- Informed Medical Decisions Foundations. Retrieved on April 27, 2012. Available at: http://informedmedicaldecisions.org
2- Stacey D, Bennett CL, Barry MJ, Col NF, Eden KB, Holmes-Rovner M, et al. Decision aids for people facing health treatment or screening decisions. Cochrane Database Syst Rev. 2010;10.
3- Arterburn D, Wellman R, Westbrook E, et al. Introducing decision aids at Group Health was linked to sharply lower hip and knee surgery rates and costs. Health Affairs. 2012. 31(9):2094-2104.
4- PT in Motion. “Decision Aids” sharply reduce hip and knee surgeries. 4. 10 (Nov 2012): 12.
images retrieved from:
http://clinic.bupa.co.uk/~/media/Images/Knee%20Decision%20Aid/pro.ashx?h=328&w=672
http://s3.amazonaws.com/content.thirdway.org/publishing/images/files/000/001/036/Impact_of_Medical_Discussion_Guides.jpg?1425396558
